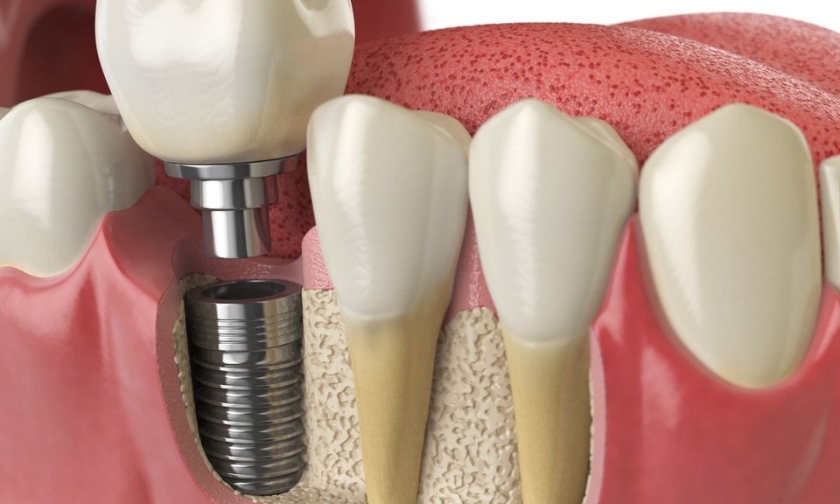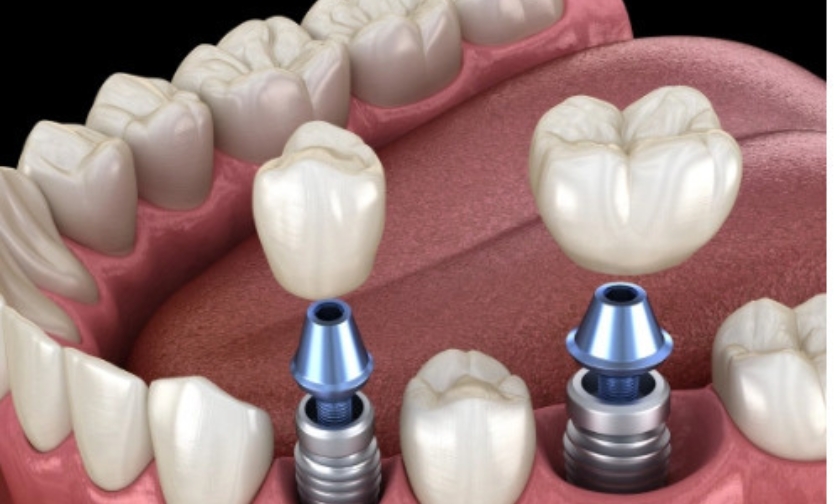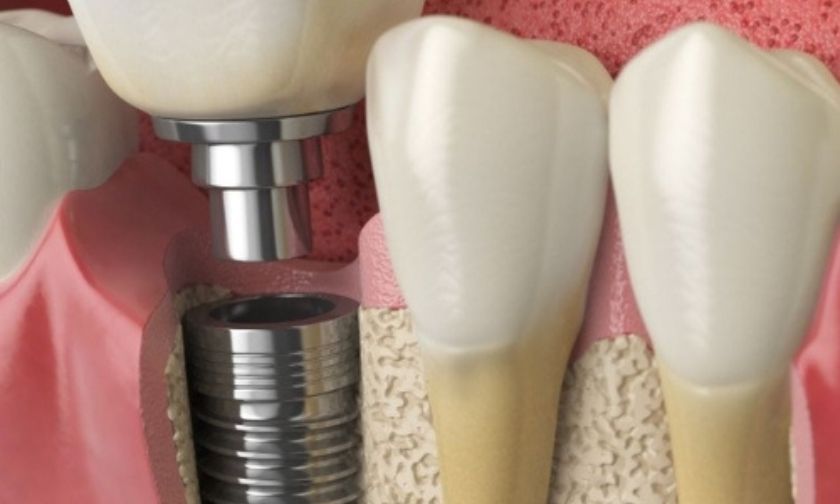
Most people considering dental implants focus on the same things: how they look, how they function, and how long they’ll last. But there’s a prerequisite that often gets overlooked — the patient’s gum health.
Ongoing gum disease and dental implants do not work together. It’s one of the most well-documented reasons implants fail, and it’s preventable when the right steps are taken before placement.
What Gum Disease Does to an Implant
To understand why treating gum disease first matters so much, it helps to know what a dental implant depends on to stay in place. A titanium post is placed directly into the jawbone, where it gradually fuses with the surrounding bone through a process called osseointegration. That fusion is what makes implants so stable, but it requires healthy bone and gum tissue to occur properly.
Gum disease disrupts both. In its earlier stage, gingivitis causes inflammation and bleeding in the gum tissue. If left untreated, it progresses to periodontitis — a deep infection that destroys the connective tissue and bone that hold teeth in place. The same bacteria responsible for this destruction don’t disappear when an implant is placed. In fact, research consistently shows that those bacteria can affect the surface of a titanium implant just as readily as they attack natural tooth roots.
The result is peri-implantitis — an infection of the tissue and bone surrounding the implant. A 2024 systematic review and meta-analysis published in Clinical Implant Dentistry and Related Research confirmed that a history of periodontitis is a significant risk factor for implant failure, greater marginal bone loss, and the development of peri-implantitis. Patients with untreated or severe gum disease face a hazard ratio for implant failure more than eight times higher than periodontally healthy patients after the four-year mark, according to a long-term cohort study in PubMed covering 2,336 implants.
For patients in the Park City and north Wichita area considering dental implants, this information is worth having before any treatment begins.
Signs You May Have Gum Disease Without Knowing It
Here’s what makes this particularly tricky: gum disease is often silent in its early stages. Many patients have no pain, no visible changes, and no reason to suspect anything is wrong. By the time symptoms like persistent bad breath, gum recession, loose teeth, or bleeding gums during brushing appear, the disease has often been progressing for months or years.
Watch for these indicators:
- Gums that bleed when you brush or floss, even lightly
- Gums that appear pulled back or lower than they used to be
- Persistent bad breath that doesn’t improve with brushing
- Teeth that look longer than before
- A change in how your bite feels
- Any tooth mobility
None of these symptoms alone confirms gum disease, but they warrant a professional evaluation before any discussion of implants moves forward. Studies show that approximately 46% of all adults aged 30 or older show signs of gum disease, meaning this is far more common than most people assume.
How Newton Dental Studio Addresses Gum Disease Before Implants
Newton Dental Studio doesn’t take shortcuts in this step, and that matters. Before any implant treatment begins, the clinical team thoroughly evaluates your gum health — probing pocket depths, reviewing digital X-rays, and assessing bone levels using cone-beam 3D imaging. This gives Dr. Davidson a complete picture of what’s happening below the gumline, not just at the surface.
If active gum disease is present, it’s treated first. The specific approach depends on how advanced the disease is.
Scaling and Root Planing
For moderate gum disease, scaling and root planing are typically the first-line treatment. This is a deep-cleaning procedure performed below the gumline, in which a clinician removes plaque, tartar, and bacterial deposits from the root surfaces of the teeth. It’s more thorough than a standard cleaning and is often done in quadrants across two or more appointments. Once completed, the gum tissue is given time to heal and reattach to the cleaned surfaces.
Periodontal Therapy and Maintenance
For patients with more advanced disease, a structured periodontal therapy program is needed before implant placement is on the table. This involves active treatment followed by more frequent maintenance visits — often every three to four months rather than the standard six — to ensure the infection is fully controlled and doesn’t return.
Soft Tissue Laser Therapy
Newton Dental Studio also uses soft tissue laser technology as part of periodontal care. The laser removes infected tissue with precision, reduces bacterial load around the gumline, and promotes faster healing than traditional methods alone. For patients managing gum disease prior to implant placement, this technology is a meaningful advantage.
Only after gum health is confirmed stable does implant planning begin. This isn’t about slowing things down — it’s about ensuring that when the implant goes in, the environment around it supports long-term success.
What Happens If You Skip This Step
It’s worth being direct about this. Placing a dental implant in a mouth with active gum disease significantly increases the risk of peri-implantitis developing around that implant. And peri-implantitis doesn’t just mean a setback — it means bone loss, potential implant failure, and a longer, more complicated recovery than would have been needed if the gum disease had been treated first.
The good news is that patients who complete periodontal treatment and commit to ongoing maintenance do very well with implants. A 20-year study published in PMC followed patients with a history of periodontitis undergoing implant therapy and found that, with proper supportive care, implant survival rates remained at 93% — comparable to those in periodontally healthy patients. The key variable was compliance with follow-up care, not the history of gum disease itself.
That’s an encouraging finding. Having a history of gum disease doesn’t disqualify you from getting implants. It means the path to implants requires one additional step — and that step genuinely changes the outcome.
What to Expect at Your Consultation
At Newton Dental Studio, the first appointment for implant consideration isn’t about rushing to a placement date. It’s a thorough evaluation of your oral health, including gum condition, bone density, bite alignment, and medical history, so that any necessary preparatory treatment is identified up front and built into the plan.
Patients from Park City, Wichita, and the surrounding north-central Kansas area come in without knowing whether they’re implant-ready. Many leave the consultation with a clear treatment sequence and a realistic timeline. For those who do need gum treatment first, that clarity is valuable — it keeps the process on track and removes the uncertainty that holds many people back from even starting.
Book a consultation at Newton Dental Studio and get a personalized evaluation of your gum health today.
People Also Ask
It depends on the severity of the disease and how well your gums respond to treatment. For mild-to-moderate cases treated with scaling and root planing, a re-evaluation typically happens six to eight weeks after treatment. If the gum tissue has healed well and pocket depths have reduced, implant planning can proceed. More advanced cases may require a longer stabilization period — sometimes three to six months — before implant placement is considered appropriate.
Yes, and this is one of the most important things to understand before committing to implants. The bacteria responsible for gum disease don’t disappear permanently after treatment. Peri-implantitis (the implant equivalent of gum disease) can develop if oral hygiene slips or if routine professional cleanings are skipped. Patients with a history of periodontal disease are advised to schedule maintenance visits more frequently than twice a year to stay ahead of any recurrence.
Almost certainly, yes. Gum disease leaves measurable clinical signs, such as increased pocket depths, bone loss visible on X-rays, gum recession, and bleeding on probing. A thorough examination at your consultation will surface these findings regardless of whether you’ve been in recently. Being upfront about any symptoms you’ve noticed helps your implant dentist put together a more complete picture from the start.
Scaling and root planing is performed under local anesthesia, so the procedure itself is generally painless. Some soreness and sensitivity in the treated area are normal for a few days afterward. At Newton Dental Studio, soft tissue laser therapy is also used, which tends to cause less post-procedure discomfort than conventional methods. Most patients manage any lingering tenderness with over-the-counter pain relief and return to normal activity the same day.
Yes. Diabetes, in particular, has a well-documented two-way relationship with periodontal disease — each condition can worsen the other. Patients managing diabetes need to be vigilant about gum health before and after implant placement. Other conditions that increase the risk of gum disease include cardiovascular disease, hormonal changes during pregnancy or menopause, and certain medications that reduce saliva flow and cause dry mouth. All of these are factors your dentist will ask about during your initial consultation.