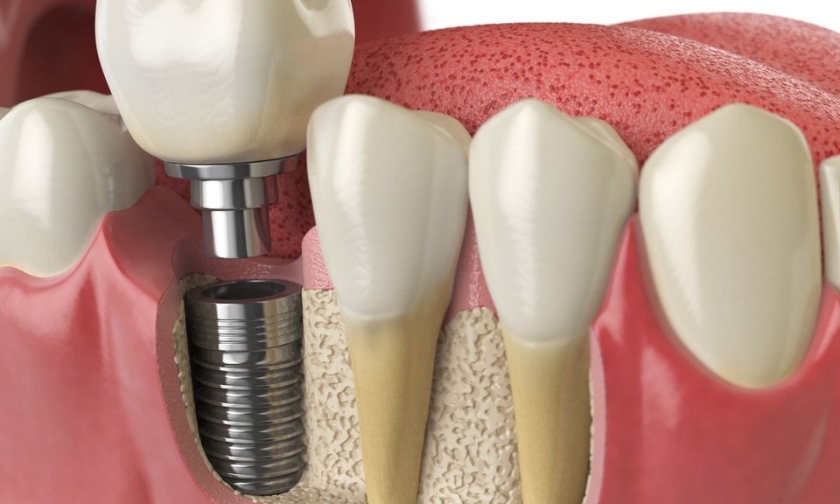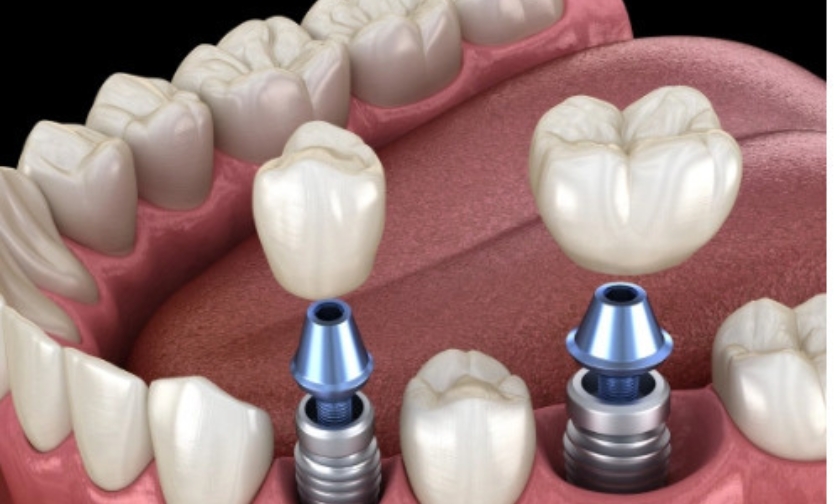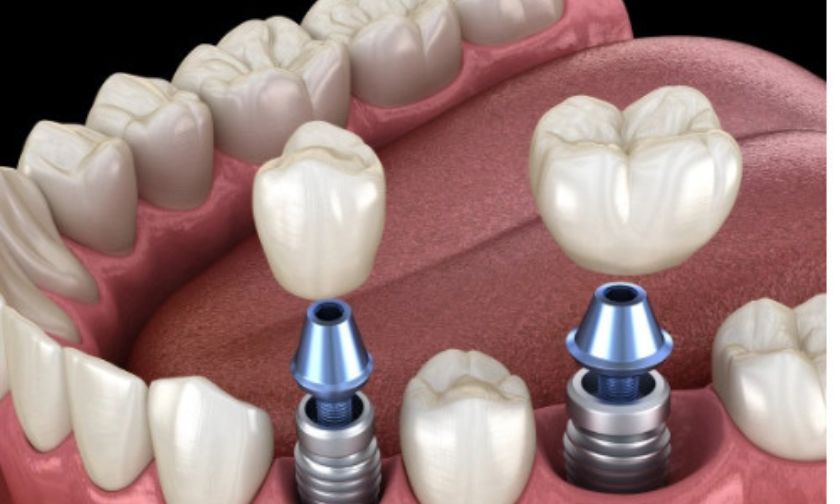
Living with an autoimmune condition is already a lot to manage. Add tooth loss to the picture, and the questions pile up fast — especially when you start wondering whether dental implants are even on the table for you. The short answer is: they often are. But the complete picture deserves a thorough conversation, not a vague “it depends.”
This blog breaks down what the research says, what factors truly matter, and what you can expect if you’re living with lupus (SLE), rheumatoid arthritis (RA), or another autoimmune disease and considering implants.
What Does the Research Say?
Here’s the reassuring part: a 2022 review published in a peer-reviewed journal analyzed 55 studies covering nine autoimmune conditions, including RA and systemic lupus erythematosus (SLE). The finding? Dental implant survival rates among patients with autoimmune diseases were comparable to those in the general population.
If you’ve been looking into dental implants in Wichita and wondering whether your diagnosis rules you out, the data leans in your favor — provided your condition is managed, and you’re working with a team that understands your medical history.
That said, success doesn’t come without conditions.
The Factors That Affect Implant Outcomes
Disease Activity and Control
Whether or not implants are right for you has a lot to do with how well-controlled your condition is — not just the diagnosis itself. Autoimmune diseases like lupus and RA are characterized by flares and remissions. Implant surgery is better planned during periods of remission, when inflammation is lower, and the immune response is more stable.
Uncontrolled disease can interfere with osseointegration — the process by which the titanium implant post fuses with your jawbone. Your body’s bone remodeling process and immune response are deeply interconnected. When that response is overactivated or unpredictably suppressed, healing becomes hard to predict.
Medications
This is one of the more nuanced aspects of implant planning for autoimmune patients, and it’s worth slowing down on.
Many people with RA or lupus take immunosuppressants like methotrexate, corticosteroids (glucocorticoids), or biologic agents. Each of these can interact with the healing process in different ways:
- Glucocorticoids have well-documented effects on bone metabolism — they promote bone loss by triggering osteoblast (bone-building cell) apoptosis. Long-term steroid use can also reduce bone density, which affects both implant candidacy and how quickly osseointegration occurs.
- Methotrexate, commonly used in both RA and lupus management, has a more debated role. Some studies suggest low-dose methotrexate doesn’t significantly impair osseointegration, while others flag it as a potential concern. It requires close coordination between your dentist and your rheumatologist to make your treatment plan functional.
- Biologic agents (like TNF inhibitors) are newer medications that suppress specific immune pathways. While case reports remain limited, caution is warranted — these drugs can increase susceptibility to infection and may affect bone healing.
Medication management around surgery is often where the planning gets detailed. Your implant dentist and rheumatologist will typically work together to time the procedure during an optimal window, sometimes adjusting medications around the day of surgery to reduce infection risk without compromising your systemic treatment.
Bone Density and Oral Health
Autoimmune conditions and the long-term medications used to treat them can affect bone density. If your jawbone density is lower than ideal, bone grafting may be recommended before or alongside implant placement. This adds steps to the process, but it doesn’t make implants impossible.
Oral hygiene also plays a larger role than many patients expect. Some autoimmune conditions cause dry mouth (a common symptom of Sjögren’s syndrome, which sometimes overlaps with RA and lupus), which increases the risk of gum disease and peri-implantitis — an infection around an implant. Additionally, joint pain and reduced hand dexterity in RA patients can make consistent oral hygiene challenging. Adaptive tools like electric toothbrushes and water flossers help bridge that gap significantly.
What Makes Implants More or Less Viable for You?
Rather than a generic yes-or-no, your candidacy comes down to a thorough evaluation. Here’s what a comprehensive assessment typically looks at:
- Current disease activity — Is your condition in remission or in an active flare?
- Medication regimen — What are you taking, at what dose, and for how long?
- Bone density — Do you have adequate jawbone structure to support an implant?
- Oral hygiene baseline — Is there existing gum disease or bone loss that needs to be addressed first?
- Coordination with your rheumatologist or specialist — Has your medical team been looped in on the plan?
If most of these check out, dental implants in Wichita are a real possibility for you — not a long shot.
What the Process Looks Like for Autoimmune Patients
The implant process for someone with lupus or RA isn’t radically different from what anyone else goes through. The key differences are in the preparation and monitoring stages.
Pre-surgical evaluation is more thorough. You’ll likely need imaging to assess bone density, bloodwork to check inflammatory markers and immune function, and a medical consultation with your rheumatologist. If bone grafting is needed, it’s completed and allowed to heal before implant placement. Healing timelines may run longer than average — that’s simply the reality of a modified immune environment, and it’s planned for accordingly.
Post-placement, the monitoring schedule tends to be more frequent. Catching peri-implant issues early is critical, and a tighter recall interval makes that possible. Many autoimmune patients go on to have implants that function well for years when the maintenance piece is treated seriously.
If you’re in the Wichita area and have been putting off this conversation because you assumed an autoimmune condition disqualified you, it’s worth getting that assumption checked.
Every patient’s situation is different, and that’s why a personalized evaluation matters more than a general answer. Newton Dental Studio works closely with patients with complex medical histories to determine the safest, most effective path to restoring their smiles. If you’re living with lupus, RA, or another autoimmune condition and want a straight answer about your options, book a consultation today.
People Also Ask
Not necessarily, and you should never adjust your medications without guidance from your rheumatologist. In many cases, medications are managed (not stopped) around the time of surgery. The goal is to minimize the risk of infection while keeping your systemic condition stable. Your implant dentist and your rheumatologist will coordinate on this together.
Yes, it can. Systemic lupus erythematosus can be associated with reduced bone mineral density, particularly in patients on long-term corticosteroid therapy. This doesn’t automatically rule out implants, but it does mean a thorough bone assessment is essential before any surgical planning begins. Bone grafting may be recommended to build up the implant site if needed.
It is a legitimate concern. Saliva plays an important role in protecting teeth and gum tissue from bacteria. Chronic dry mouth (common in Sjögren’s syndrome) often co-occurs with RA and lupus, increasing the risk of gum disease and peri-implant infections. Proactively managing dry mouth with your care team can significantly reduce this risk.
There’s no universal cutoff, but your rheumatologist can assess your current inflammatory markers (such as CRP and ESR) and provide a clinical assessment of your disease activity. Most implant dentists prefer to proceed when the condition is in remission or at a low level of disease activity. This is a conversation worth having with both your rheumatologist and your dentist.
Yes. For patients who have lost multiple teeth or have significant bone loss, implant-supported full-arch restorations (sometimes called All-on-4 or full-arch implants) may be a practical option. These require fewer implant posts placed in areas of higher bone density, which can reduce the complexity of the procedure for patients with bone density concerns.